Microbiology of SARS CoV2 amid School Re-opening – Mr. Arthur-Mensah Jnr & Dr Abigail Kyei
MICROBIOLOGY OF SARS CoV2 AMID SCHOOL REOPENING
Download PDF: Microbiology of SARS CoV2 amid school reopening
Reginald Arthur-Mensah Jnr (Department of Nursing and Midwifery, Pentecost University).
Abigail Agartha Kyei (Department of Nursing and Midwifery, Pentecost University).
Introduction
The World Health Organization (WHO) declared a global health emergency of international concern on January 30, 2020, due to the novel coronavirus disease which is caused by the SARS CoV2 virus. On February 11, 2020, WHO announced a name for the new coronavirus disease as COVID-19. On March 12, 2020, the disease was declared a pandemic1. To curb the spread of the disease in Ghana, on March 15, 2020, the government announced a series of comprehensive measures, including the closure of all schools; Basic, Junior High, Senior High and Universities. This move negatively affected some 9.2 million basic school students (kindergarten, primary and junior high schools) and 1 million tertiary education students2. Ongoing terms/semesters/trimester were interrupted and upcoming terms/semesters/trimester cannot begin until they are adapted to the new reality.
As of 6th May 2020, UNESCO estimated that 192 countries have temporarily closed schools worldwide, impacting over 1.6 billion learners globally2. The scale and speed of school closures were unprecedented worldwide. Never before had so many students been out of school at the same time, disrupting learning and upsetting visions of the youth. School closures were based on evidence and suggestions from the previous influenza outbreaks that they reduce physical contacts between persons and therefore interrupt transmission of infections3.
There is an urgent need to identify how countries can safely return students to school and parents to work once the number of COVID-19 cases begins to fall. The decision to reopen schools for in-person educational instruction is among the greatest challenges of many governments. Around the world, this has become a contentious issue, with students, their families, and educators expressing strong opinions about what is best for them. There has never been a more important time for open discussion and collaboration with the goal of reaching a consensus on the reopening of schools while protecting the health and well-being of students and educators during the COVID-19 pandemic.
The best way to avert and slow down transmission in the midst of school reopening is to be well informed about the characterization of the COVID-19 virus, how it spreads from one source to another, the pathogenesis of the disease, the pathophysiology of the disease and how it can be prevented. Be that as it may, the pandemic is expected to have significant long-term effects on education.
Characteristics in Coronaviruses
Coronaviruses (CoVs) are enveloped, positive-sense, single-stranded RNA viruses that belong to the subfamily Coronavirinae, family Coronaviridiae, order Nidovirales. There are four genera of CoVs, namely, Alphacoronavirus (αCoV), Betacoronavirus (βCoV), Deltacoronavirus (δCoV), and Gammacoronavirus (γCoV)4. Evolutionary analyses have shown that bats and rodents are the gene sources of most αCoVs and βCoVs, while avian species are the gene sources of most δCoVs and γCoVs4. CoVs have repeatedly crossed species barriers and some have emerged as important human pathogens. The best-known examples include severe acute respiratory syndrome CoV (SARS-CoV) which emerged in China in 2002–2003 to cause a large-scale epidemic with about 8000 infections and 800 deaths, and Middle East respiratory syndrome CoV (MERS-CoV) which has caused a persistent epidemic in the Arabian Peninsula since 20125.
Prior to December 2019, 6 CoVs were known to infect human, including 2 αCoV (HCoV-229E and HKU-NL63) and 4 βCoV (HCoV-OC43 [lineage A], HCoV-HKU1 [lineage A], SARS-CoV [lineage B] and MERS-CoV [lineage C]). The βCoV lineage A HCoV-OC43 and HCoV-HKU1 usually cause self-limiting upper respiratory infections in immunocompetent hosts and occasionally lower respiratory tract infections in immunocompromised hosts and the elderly5. In contrast, SARS-CoV (lineage B βCoV) and MERS-CoV (lineage C βCoV) may cause severe lower respiratory tract infections with acute respiratory distress syndrome and extrapulmonary manifestations, such as diarrhoea, lymphopenia, deranged liver and renal function tests, and multiorgan dysfunction syndrome, among both immunocompetent and immunocompromised hosts with mortality rates of ∼10% and ∼35%, respectively6
SARS-CoV2 has a diameter of 60 nm to 140 nm and distinctive spikes, ranging from 9 nm to 12 nm, giving the virions the appearance of a solar corona (see Figure 1). Bats are thought to be a natural reservoir for SARS-CoV2, but it has been suggested that humans became infected with SARS-CoV2 via an intermediate host, such as the pangolin7.
Generally, coronaviruses cause respiratory, gastrointestinal and neurological disease8.
Transmission of SARS-CoV2
Human respiratory droplets expelled during face-to-face exposure during talking, coughing, or sneezing is the most common mode of transmission. Prolonged exposure to an infected person i.e. being within 6 feet for at least 15 minutes and briefer exposures to individuals who are symptomatic (e.g., coughing) are associated with a higher risk for transmission, while brief exposures to asymptomatic contacts are less likely to result in transmission9. Contact surface spread i.e. touching a surface with SARS CoV2 on it is another possible mode of transmission8. Transmission may also occur via aerosols i.e. smaller respiratory droplets that remain suspended in air, but it is unclear if this is a significant source of infection in humans, however, it is associated with the low-risk transmission of the virus10.
Pathogenesis of SARS-CoV2
Upon contact with the virus from an infected source through any of the routes of transmission, the virus enters the human host cell. To be successful, the virus targets human host cells, such as nasal cells (relating to the cells that line the nose), bronchial epithelial cells (relating to cells that line the bronchus) and pneumocytes (relating to the cells that line the alveoli)8. They attach to these cells through the viral structural spike, (S) protein (see Figure 1) that binds to the angiotensin-converting enzyme 2 (ACE2) receptor. After binding, the type 2 transmembrane serine protease (TMPRSS2), present in the human host cell promotes viral uptake into the cells by cleaving ACE2 and activating the SARS-CoV2 S protein (see Figure 2A). Activation of the S protein mediates the virus to enter the host cells through endocytosis. Endocytosis is the process by which the cell membranes of a cell folds inwards to ingest the material. This mechanism is possible through the receptor-binding domain (RBD) between SARS-CoV2 S proteins and ACE2 and TMPRSS2 human host target cells. These human host receptors are particularly expressed in alveolar epithelial type II cells (cells of the tiny air sacs of the lungs)11.
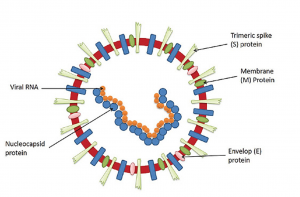
Figure 1: Structural details of SARS CoV212
Pathophysiology of SARS-CoV2
On entry, viral replication begins. The viral inflammatory response, consisting of both the innate and the adaptive immune response i.e. comprising the humoral and cell-mediated immunity, impairs lymphopoiesis i.e. the formation of lymphocytes in the bone marrow, lymph nodes, thymus and spleen and increases lymphocyte apoptosis i.e. a type of cell death in which the cell uses specialized cellular machinery to kill itself. As such, profound lymphopenia i.e. an abnormally small number of lymphocytes in the circulating blood may occur. This allows the virus to infect and kill T lymphocyte cells of the host8 (see Figure 2B).
As viral replication, transcription and translation accelerate and infection continues, the epithelial-endothelial barrier integrity of the alveolar is compromised (see Figure 2C). In addition to the epithelial cells, the virus infects pulmonary capillary endothelial cells, heightening the inflammatory response and triggering an influx of monocytes and neutrophils into the alveolar. Interstitial mononuclear inflammatory infiltrates and edema i.e. swelling from excessive accumulation of watery fluid in cells, tissues, or serous cavities, develop and appear as ground-glass opacities on computed tomographic (CT) imaging. Pulmonary edema filling the alveolar spaces with hyaline membrane formation follows, compatible with early-phase acute respiratory distress syndrome (ARDS). Bradykinin-dependent lung angioedema may also contribute to the disease13. Collectively, endothelial barrier disruption, dysfunctional alveolar-capillary oxygen transmission, and impaired oxygen diffusion capacity are characteristic features of COVID-198.
Further, fulminant (sudden and severe) activation of coagulation and consumption of clotting factors occur leading to diffuse intravascular coagulation. Inflamed lung tissues and pulmonary endothelial cells may result in the microthrombi formation and contribute to the high incidence of thrombotic complications, such as deep venous thrombosis, pulmonary embolism and thrombotic arterial complications such as limb ischemia, ischemic stroke, myocardial infarction in critically ill patients. The development of viral sepsis, defined as life-threatening organ dysfunction caused by a dysregulated host response to infection may further contribute to multiorgan failure including the heart, brain, lung, liver, kidney and the coagulation system14.
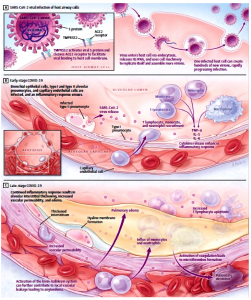
Figure 2: Pathogenesis and pathophysiology of SARS CoV28
Symptoms of COVID-19
COVID-19 affects different people in different ways. Averagely, it takes 5 – 6 days from when someone is infected with the virus for symptoms to show, however it can take up to 14 days. Most infected people will develop mild to moderate illness and recover without hospitalization. Some may also develop severe complications of the disease or other comorbidities and death may result. Currently, the most serious symptoms include difficulty breathing or shortness of breath, chest pain or pressure and loss of speech or movement. Most common symptoms include fever, dry cough and general fatigue. The fewer common symptoms are aches and pains, sore throat, diarrhoea, conjunctivitis, headache, loss of taste or smell, a rash on skin and discolouration of fingers or toes15.
School reopening
As students prepare to come to school, it is cardinal for both educators and students to adhere to the following precautionary and preventive measures against the ongoing pandemic.
- The regular washing of hands with soap under running water before and after lectures
- The intermittent sanitizing of the hands with an alcohol-based hand rub during a lecture
- Avoidance of touching the T zone of the face as well as the eyes, nose and mouth
- Wearing of face protection e.g. nose masks, face shields at all times on return to campus
- Practising physical distancing in the classrooms, social gatherings and staying away from crowds and large groups of people.
- Refraining from smoking and other activities that weaken the lungs.
- Staying home if one feels unwell.
Moreover, general school infection prevention and control practices should be enforced more effectively at this time.
Education is one of the strongest predictors of the health and the wealth of a country. Giving schools the support they need to confront COVID-19 could result in safe, healthy, and thriving environments for students and ultimately recognize education as a critical determinant of development in countries.




